Learning Outcomes:
Diseases caused by these major pathogen groups include
Tuberculosis (pp.440-442)
- Tuberculosis (TB) is caused by the bacteria Mycobacterium tuberculosis
- Most often effects the lungs, occasionally spreads to lymph glands, bones, joints, kidneys and many other areas.
- 25% of the worlds population have a latent infection .
- TB is spread via airborne transmission.
- Can only be contracted by a person with active tuberculosis.
- Only 10% of latent infections become active.
- 50% mortality rate once active phase is reached
- At the early stage the body's defense system may fight off the infection and will not show symptoms (they have "latent" tuberculosis).
- If the body is not successful, the bacteria multiplies and symptoms form.
- The disease turns into what's called active tuberculosis, rather than latent TB.
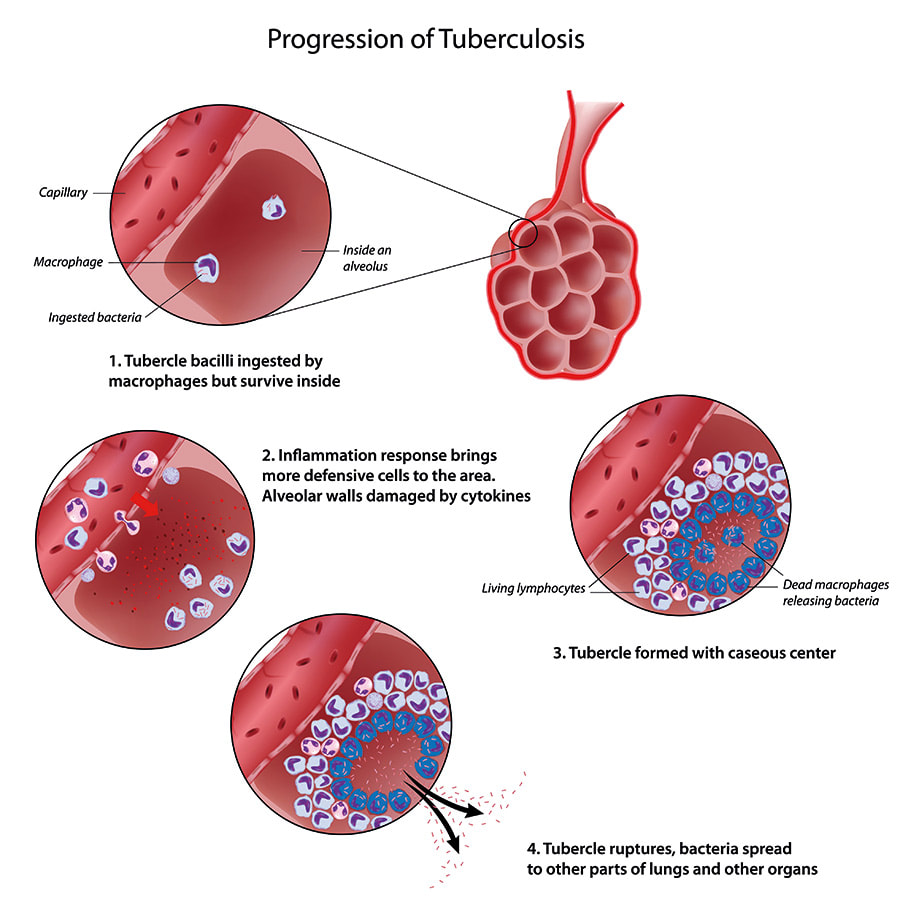
- Onset 1-7 Days: The bacteria is inhaled.
- 7-21 Days: If the bacteria does not get killed then it reproduces.
- 14-21 Days: Tuberculosis starts to develop when the bacteria slows down at reproducing, they kill the surrounding non-activated macrophages and run out of cells to divide in. The bacteria then produces anoxic conditions and reduces the pH. The bacteria can't reproduce anymore but can live for a long time.
- After 21 days: Macrophages surround the tubercule. Tuberculosis then uses it to reproduce which causes it to grow. The turbecule can break off and spread around. If it spreads in the blood you can develop tuberculosis outside the lungs.
- Liquification and Cavity Formation: The tubercules at one point will liquify, which will make the disease spread faster. Only a small percent of people will get to this stage.
- Newly arrived immigrants or refugees have an increased risk
- People with poor nutrition, severe illness or drink alcohol excessively.
- Poverty and TB are closely linked
- Young children, especially if they are malnourished
- Marginalized or disadvantaged (avoid using health clinics out of fear that their family will reject them if diagnosed)
- Persistent cough, lasting for more than three weeks
- Fever
- Loss of energy
- Sweats
- The cough may produce phlegm and sometimes blood
- Unexplained weight loss
- Chills
- Loss of appetite
Treating Tuberculosis
- Latent TB:
- Daily dose of antibiotics for 6 to 9 months.
- Active TB:
- Antibacterial medication for 6 to 12 months.
- Failure to take the full course of medications can lead to drug-resistant TB that is much more difficult to treat.
Why is it difficult to control the spread?
- In developing countries it may takes weeks before a case is confirmed in a medical laboratory - meaning hygiene and isolation practices are not put in place in time.
- In developing countries, infected people may not have access to medical help
- TB vaccines do not work effectively for all adults
- TB has a low infective dose of just 10 bacteria to estabilsh itself in human lungs
- If bacteria become active, the syptoms are delayed, delaying hygiene practices and increasing likelihood of tranismssion.
- Most people are susceptible to the disease - especially those with weakened immune systems.
- Developing countries have a greater number of people with weakened immune systems thus a greater susceptibility to TB
- Drug resistent strains of TB have developed to the point where there is little improvement in recent years in the incidence of the disease.
- Inadeqate education about the disease and its transmission (especially in developing countries) means people are more likely to spread TB and less likely to seek medical treatment.
Population Density and TB
- Higher the density the higher the rate of infection/transmission.
- In regions with a high population density the rate and transmission of TB is extremely high.
- One third of the world’s population is infected with TB.
- TB is a leading killer of people who are HIV infected.
Tetanus (pp.442-443)
What is tetanus?
Tetanus Symptoms
Tetanus Life Cycle
Treatment:
Prevention:
- Tetanus is a bacterial disease that causes muscle spasms and breathing problems.
- Tetanus is caused by the bacteria Clostridium tetani
- Tetanus is transmitted indirectly (cannot be passed from human to human contact)
- A person can become infected when dirt (particularly rust) enters a wound.
- The bacteria grows in wounds caused by dirty nails, knives, tools, wood splinters, and animal bites.
- The toxins released by the bacteria cause life-threatening symptoms
Tetanus Symptoms
- Muscle spasms (start in the jaw and neck)
- Inability to open the mouth (lockjaw due to muscle stiffness)
- Difficulty swallowing
- Breathing difficulties
- Painful convulsions (fits)
- Abnormal heart rhythms
- Fever
- High blood pressure
- Sweating
- Newborn babies with tetanus are normal at birth, but stop sucking between three and 28 days after birth. They stop feeding and their bodies become stiff while severe muscle contractions and spasms occur. Death follows in most cases.
Tetanus Life Cycle
- C. tetani enters the host through a break in the skin (such as a wound), where it then replicates.
- Tetanus toxin is generated in living bacteria, and is released when the bacteria lyse, such as during spore germination or vegetative growth.
- The bacteria cannot grow or reproduce when oxygen is present.
- When its exposed to air, it forms protective spores that lie dormant.
- The spores can remain in soil for years as they are resistant to heat, desiccation and UV radiation.
- Minimal amount of spore germination and vegetative cell growth are required for toxin production.
- The bacteria can be reactivated when the conditions are favourable for growth.
- After entering the host cell, C. tetani produces two exotoxins; tetanolysin and tetanospasmin.
- The purpose of Tetanolysin is unknown.
- Tetanospasmin is a neurotoxin that causes tetanus.
- Tetanospasmin circulates in the body where it invades the central and peripheral nervous system.
- This causes the neurotransmitters to be inhibited where muscle contraction and spasms can occur.
Treatment:
- Antitoxin tetanus immunoglobulin) – to neutralise any tetanus toxin that is circulating and not yet attached to nerve tissue
- Anti-convulsive medications
- Antibiotics – to prevent multiplication of Clostridium tetani, preventing production and release of toxins
- Sedative/hypnotic agents – treat muscle spasm, rigidity and tetanic seizures.
Prevention:
- Vaccinations every 5-10 years.
- Immunising infants and children.
- Immunising pregnant women can prevent neonatal tetanus (tetanus in newborn babies).
- Clean practices are especially important when a mother is delivering a child, even if she has been immunised.
- Elimination and eradication of tetanus is not possible as it exists in the environment.
- The percentage of pregnant women being immunised needs to increase.
- Administer tetanus toxoid to all women of childbearing age.
- Promote clean delivery and childcare practices.
- To be protected, an individual should receive 3 doses of DTP in infancy, followed by a TT-containing booster at school-entry age (4-7 years), in adolescence (12-15 years), and in early adulthood.
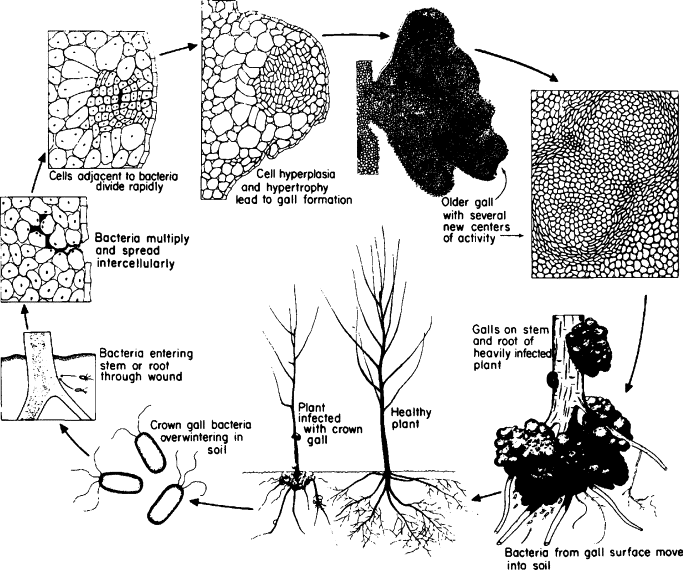
Crown Gall (pp.443-444)
|
Transmission:
- The woody galls that have previously infected an organism, fall to the ground to invade other organisms near it
- It has an indirect mode of transmission,
- Requires a puncture in the root system in order to infect the host.
- Plant cells that have been damaged by insects or animals release chemical signals into the soil, attracting Agrobacterium.
- If there is a large host population density in the area, they can be severely affected by the crown gall pathogen.
- The pathogen doesn’t need a high host population density as it can travel through water ways and soil for more than 3 years.
- Reproduces via inserting sections of it’s DNA and retreating back to the soil once a secondary invader takes it’s place in the infected plant.
Managing Crown Gall:
- The plant must be carefully dug up and destroyed
- Do not replace with another susceptible plant in the same site for years after, as crown gall can last in the soil for more than 2 years
- Sterilize pruning tools via heating or chemically treating the tools
- There is a chemical treatment for the removal of Crown Gall bacterium mostly used in commercial business’ due to the high cost of completing the treatment