Learning Objectives
The spread of a specific disease involves a range of interrelated factors, including
Transmission and spread of disease is facilitated by regional and global movement of organisms (SU)
The distribution of mosquito-borne diseases may be affected by global climatic changes (SU)
Many pathogens evolve rapidly in a changing environment (SU)
Management strategies are used to control the spread of infectious diseases, including
The life cycle of a pathogen and its associated diseases, including the method of invading the host, the impact on the host, and the mode of transmission (direct or indirect), determines its success for survival (SU)
- growth of the pathogen population
- density of the host population
- mode of transmission (SU)
Transmission and spread of disease is facilitated by regional and global movement of organisms (SU)
The distribution of mosquito-borne diseases may be affected by global climatic changes (SU)
Many pathogens evolve rapidly in a changing environment (SU)
Management strategies are used to control the spread of infectious diseases, including
- quarantine,
- immunisation – herd immunity,
- disruption of pathogen life cycle,
- medications – antibiotics and antivirals,
- physical preventative measures (SU)
The life cycle of a pathogen and its associated diseases, including the method of invading the host, the impact on the host, and the mode of transmission (direct or indirect), determines its success for survival (SU)
THREE KEY STEPS FOR DEALING WITH DISEASE:
Break the cycle of transmission
Kill the infectious agents
Increase host resistance
Break the cycle of transmission
Kill the infectious agents
Increase host resistance
Growth of pathogen population
Pathogens that can replicate quickly will spread more easily
- As a result, bacterial pathogens are more widely spread than diseases like malaria that require a vector
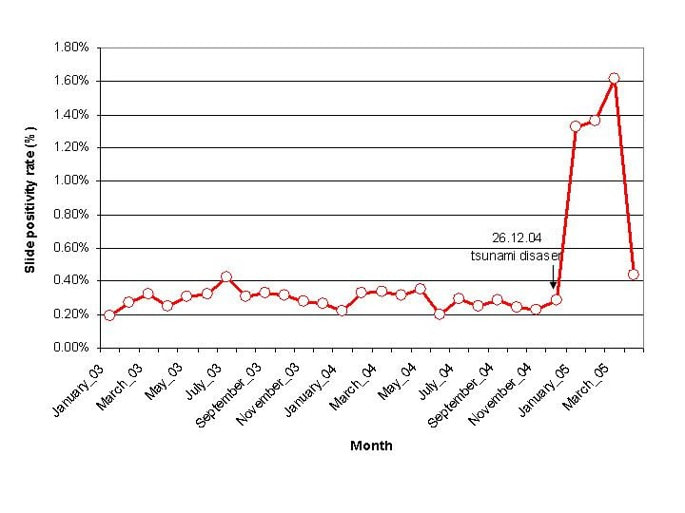
- After disasters/disturbances, sanitation is often reduced and waste more prolific, this facilitates pathogen growth
- Standing water promotes mosquito, bacterial, fungal and protist growth
- Mosquitoes prefer warm and wet conditions - thus climatic changes, tsunamis, tropical cyclones, or any other cause for a more wet and warm environment can result in a Malaria outbreak.
- Climate change to warmer temperatures increase lifecycle of many pathogens (e.g. plasmodium) resulting in increased prevalence
Density of host population
- A high population density means an increased risk of an epidemic
- Disease spreads more quickly in a dense population
- In an epidemic, many people are infected, in a pandemic there are many infected people in a large geographic area.
- High-density populations mean a greater likelihood of close contact thus a quicker spread of disease
- Density issues can be abated or minimised by vaccination rates, herd immunity and healthcare access
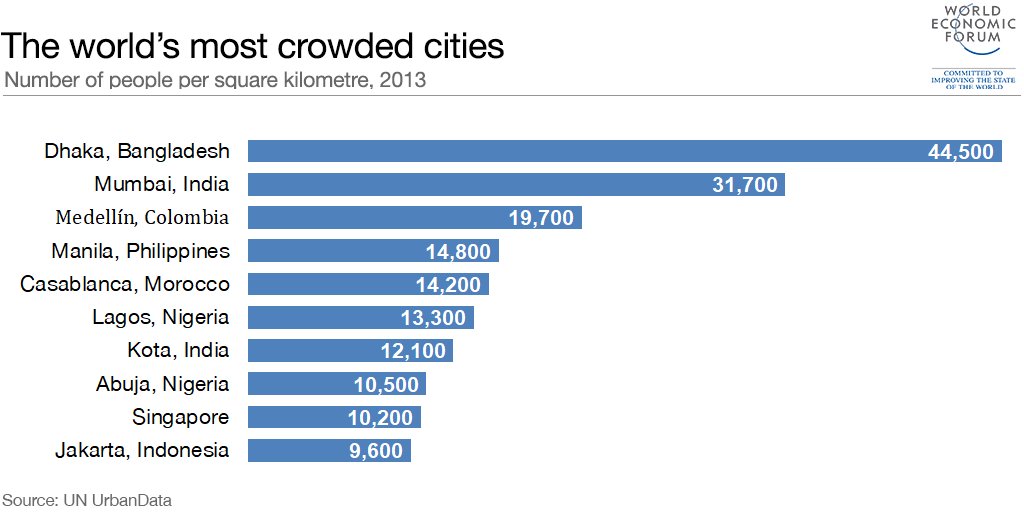
COVID-19 as an example...
Dhaka: Recorded 58% of Bangladesh's COVID-19 cases despite accounting for only 5.5% of the nation's total population
Mumbai: more than 20% of India's COVID-19 cases despite accounting for only 1% of the nation's population
Dhaka: Recorded 58% of Bangladesh's COVID-19 cases despite accounting for only 5.5% of the nation's total population
Mumbai: more than 20% of India's COVID-19 cases despite accounting for only 1% of the nation's population
Modes of transmission:
- Diseases are transmitted at differing rates in a population
- The transmission rate is partly determined by the mode of transmission
- For example,
- Ebola is believed to be spread easily by direct contact and indirect contact (with contaminated objects)
- HIV is only spread through sexual contact, blood transusions and mother-baby placenta and breastfeeding.
- Thus contracting Ebola is more likely than contracting HIV due to the ease of transfer of Ebola
- The means by which a pathogen enters and the organs it targets also affect transmission rate.
- For example
- Ebola enters its host via mucose membranes (eyes, nose, digestive tract and sexual organs.
- Tetanus can only enter through an open wound.
Increased Host Resistance
- Since many of these diseases require a host for reproduction, this ensures hosts can kill pathogens and thus forces a break in their life cycle.
- This can be achieved by:
- Greater administration of vaccinations
- Makes more people immune to the disease.
- Protects the most vulnerable (saves lives).
- Fewer people will be infected as it essentially decreases the denisity of viable hosts (herd immunity).
- Greater administration of vaccinations
- Quarantine
- Isolating infected individuals or mediums to prevent spread of disease to new hosts
- prevents spread of pathogens across political boundaries
- To be effective:
- Needs to be well advertised or well supported by the public
- Needs to have serious consequences for breaches of quarantine
- Needs to be well enforced
- Needs borders to be well managed (difficult to cross without permission)
- Immunisation – (Herd Immunity)
- Immunisation also protects indivudals that have not been immunised
- Herd immunity occurs when a large percentage of a population is immune
- immunity via vaccination
- immunity via having recovered from the disease
- Herd immunity means that most individuals will not get infected.
- Thus, there is less chance of a non-immune (or unvaccinated) individual coming in contact with an infected and contagious individual.
- The greater the proportion that are vaccinated/immune, the greater the protection for those who are not.
- Disruption of pathogen life cycle E.g.
- target vector species to limit breeding populations (e.g. insecticide use on mosquitoes)
- Cover up to reduce insect bites
- Improve sanitisation and hygiene to prevent pathogens from breeding
- anti-malarial drugs
- antiviral drugs (distrupt life cycle by inhibiting the virus' uncoating and synthesis and release of new particles)
- Physical preventative measures
- Better sanitation and hygiene practices.
- covering coughs and sneezes
- handwashing
- social distancing
- Prevents spread of pathogen to new hosts
- Better sanitation and hygiene practices.
- Access to medication
- Antibiotics
- Work on bacteria only
- Reduce the risk of infections spreading
- Targets bacterial processes such as cell wall, protein and DNA synthesis
- Can cause bacterial cell lysis
- Resistance to antibiotics is common, often a result of misuse of antibiotics.
- Antivirals
- Work on viruses only
- Interrupts viral life cycle by inhibiting uncoating and the synthesis and release of more particles.
- Shortens the time in which a host is contagious
- Resistance to antivirals is rare
- Antibiotics
Evolution of pathogens
Food for thought...
Medical health experts recommend an annual influenza vaccine...why?
Some are harmful and others are beneficial, while the rest have no apparent effect.
When harmful microorganisms enter our bodies, a battle begins.
Rapid reproduction and natural selection
Medical health experts recommend an annual influenza vaccine...why?
- Flu viruses evolve rapidly.
- As they circulate around the world and switch hosts, flu viruses change
- They evolve so much that out vaccines are rendered obsolete every year
Some are harmful and others are beneficial, while the rest have no apparent effect.
When harmful microorganisms enter our bodies, a battle begins.
Rapid reproduction and natural selection
- Because bacteria and viruses reproduce rapidly, they evolve rapidly.
- Short generation times (some bacteria have a generation time of just 15 minutes)
- Thus natural selection acts quickly.
- In each pathogen generation, new mutations and gene combinations are generated
- These mutations then pass through the "selective filter" of our drugs and immune response.
- Over the course of many pathogen generations (maybe just a week or so!), they adapt to our defenses!
- This sort of rapid evolution can take place under other changes as well such as changing climates, mediums or host species.